
 |
Proliferative Retinopathy |
 |
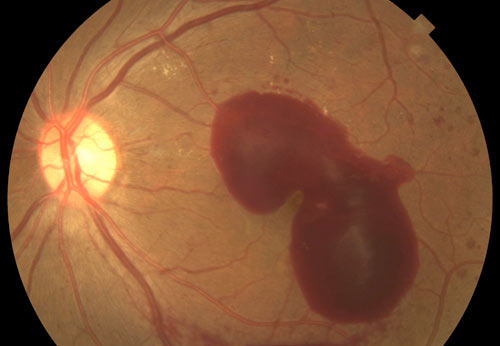
Proliferative Retinopathy | ||
When diabetic retinopathy progresses, the signs and symptoms of non-proliferative diabetic retinopathy are worsened by the addition of new abnormal blood vessels forming in the periphery of the retina. The abnormal vessels may move further into the retina and impact the macula and the optic disc. There may also be fibrovascular activity that causes pulling on the retina that further distorts the vision and can lead to worsened diabetic macular edema and a tractional retinal detachment. | ||
| ||
A long history of diabetes, often uncontrolled, leads to proliferative diabetic retinopathy. | ||
| ||
Depending on the amount of abnormal vessel growth, fibrovascular activity and the location of it in the retina, the vision impact can be anything from distortion to blindness. | ||
| ||
Diabetic retinopathy is diagnosed by retinal examination, special pictures called a fluorescein angiogram, an OCT (optical coherence tomography) scan and sometimes an ultrasound of the eye. | ||
| ||
Moderate to severe diabetic retinopathy may require injections of medication to the eye, laser treatments in the retina, or in some cases surgery. Following your doctor’s recommendations is essential to preserving eyesight. | ||
| ||
Maintaining a Hemoglobin A1C level of 7.0 or below will help prevent diabetic retinopathy from advancing to severe stages. Having regular retina examinations and any necessary treatments will help maintain your vision once diabetes has impacted your eyesight. | ||
| ||
 |
 |
|
